创伤患者:我们需要院前气管插管吗?
2016-04-14 文章来源:骨科在线 我要说
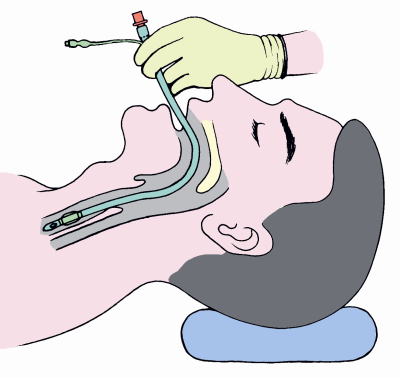
基础方面
基于大鼠的失血性休克模型研究结果显示:院前气管插管与未行院前气管插管死亡率无差异,与纯氧面罩吸氧相比,院前气管插管正压通气可造成静脉回流减少,加剧终末器官低灌注。而基于猪的一项失血性休克模型研究结果显示:院前气管插管与未行院前气管插管死亡率无差异,与纯氧面罩吸氧相比,院前气管插管组血乳酸水平更高,体温更低,失血量更大。
临床方面
《内科学年鉴》2015年10月13日发布观察性研究论文结果报告:创伤患者中,院前ALS组90天存活率低于院前BLS组。一项研究显示,院前气管插管对于单纯TBI来说,死亡率(校正混杂因素后)更高,入院时氧和更差。2013年的一项观察性研究发现严重TBI患者(GCS<8分)基本气道管理组GOS评分在4-5分组者比气管插管组高。Chou等回顾性分析了2012年1月至2014年6月洛杉矶创伤系统数据库中552例接受大量输血的创伤失血性休克患者的相关数据,其中63例接受现场气管插管,其余489例未给予现场气管插管。与未经现场气管插管组相比,现场气管插管组GCS评分(3vs.14,P<0.001)和收缩压更低(86vs.104,P<0.001),ISS评分更高(41vs.29,P<0.001),死亡率更高(83%vs.43%,P<0.001)。两组年龄、性别、钝性伤比例、现场时间、输血类型等的差别无统计学意义。校正混杂因素后,现场气管插管的患者增加死亡风险(AOR 2.89;95% CI 1.08-7.78, P=0.035),现场气管插管构成死亡的独立危险因素(AOR 3.41;95% CI 1.35-8.59, P=0.009)。作者认为采用侵入性更低的气道干预手段和快速转运或能提高这些患者的预后。基于德国创伤数据库的研究结果显示,院前气管插管与院前治疗时间延长有关。院前气管插管并不能降低穿透性创伤患者的并发症(脓毒症、肺部并发症、DVT、创面感染等),穿透伤患者院外高级生命支持无益。
最可能需要进行院前气管插管的患者包括心脏骤停、慢性肺疾病、严重创伤性休克后。但正压通气所带来的心血管负面影响对于这些患者来说也是极具危险性的。法国人的一项包含1251例院前气管插管资料显示,气管插管并发症可高达13%,包括导管误入食道,氧饱和度降低,主支气管插管,误吸,呕吐,支气管痉挛,喉痉挛等。这些并发症更多的发生于插管困难者、喉镜检查分级(Cormack-Lehane分级)>1、超重。训练有素的院前急救人员可以提高插管成功率,可视喉镜的应用也可改善插管成功率。尽管如此,近三年的证据不支持创伤患者进行院前气管插管。
参考文献
1.Taghavi S etal. Still making the case against prehospital intubation: a rat hemorrhagicshock model. J Trauma Acute Care Surg. 2012 Aug;73(2):332-7.
2.Taghavi S et al. Examining prehospitalintubation for penetrating trauma in a swine hemorrhagic shock model. J TraumaAcute Care Surg. 2013 May;74(5):1246-51.
3.Chou D, Harada MY, Barmparas G, et al.Field intubation in civilian patients with hemorrhagic shock is associated withhigher mortality. J Trauma Acute Care Surg. 2015 Oct 21.
4.Wyen H et al. The golden hour of shock- how time is running out: prehospital time intervals in Germany--amultivariate analysis of 15, 103 patients from the TraumaRegister DGU(R). Emerg Med J. 2013 Dec;30(12):1048-55.
5.Sanghavi P etal.Outcomes of Basic Versus Advanced LifeSupport for Out-of-Hospital MedicalEmergencies. Ann Intern Med. 2015 Oct 13.
6.Karamanos E etal. Is prehospital endotracheal intubation associated with improvedoutcomes in isolated severe head injury? A matched cohort analysis. PrehospDisaster Med. 2014 Feb;29(1):32-6.
7.Taghavi S etal.Prehospital intubation does not decreasecomplications in the penetrating trauma patient. Am Surg. 2014 Jan;80(1):9-14.
8.Seamon MJ etal.Prehospital interventions forpenetratingtrauma victims: a prospective comparison between Advanced LifeSupport and Basic Life Support. Injury.2013 May;44(5):634-8.
Pepe PE et al. Prehospitalendotracheal intubation: elemental or detrimental? Crit Care. 2015;19:121.
9.Caruana E et al. Trachealintubation related complications in the prehospital setting.Emerg Med J. 2015Nov;32(11):882-7.
10.Jarvis JL et al. EMSIntubation Improves with King Vision Video Laryngoscopy. Prehosp Emerg Care.2015 Oct-Dec;19(4):482-9.
11.Thoeni N et al. Incidence of difficult airwaysituations during prehospital airway management by emergency physicians--aretrospective analysis of 692 consecutive patients. Resuscitation. 2015May;90:42-5.
12.Al-Thani H et al. Prehospitalversus Emergency Room Intubation of Trauma Patients in Qatar: A-2-yearObservational Study. N Am J Med Sci. 2014 Jan;6(1):12-8.
13.McQueen C et al. Prehospital anaesthesiaperformed by physician/critical care paramedic teams in a major trauma networkin the UK: a 12. 14.month review of practice. Emerg Med J. 2015 Jan;32(1):65-9.
15.Sobuwa S et al. Outcomes followingprehospital airway management in severe traumatic brain injury. S Afr Med J.2013 Jul 29;103(9):644-6.


 京公网安备11010502051256号
京公网安备11010502051256号