Minimally Invasive Reconstruction of The Lateral Ankle Ligaments Using Semitendinosus Autograft or Tendon Allograft
2014-12-17 文章来源:徐向阳 胡牧 我要说
ABSTRACT
Objective:To retrospectively compare thetherapeutic effect between semitendinosus autograft and tendon allograft usedfor lateral ankle ligaments reconstruction.
Materials and Methods: From September 2006 to June 2011, 68patients (41 males, 27 females) with chronic ankle instability underwent anatomical reconstructionsof the lateral ligaments using semitendinosus autograft (autograft group, 32 patients) or tendon allograft(allograftgroup, 36 patients) via a minimallyinvasive approach.Allpatients were followed up for at least 12 months. The American Orthopaedic Foot and AnkleSociety Ankle Hindfoot Scale score (AOFAS score) and stress tests were used to evaluate the clinicaloutcomes and patientsatisfaction. Besides, the operation time, fever days and time toheal were also recorded.
Results: The averageoperation time was significantly increased in autograft group compared withallograft group (85.5 ± 11.5 min vs. 58.1 ± 10.2 min, P = 0.0000). However, thefever days and time to heal were significantly longer in allograft group (5.5 ±1.5 days vs. 2.5 ± 1.2 days, P = 0.0000; 13.5 ± 5.2 months vs. 11.2 ± 4.1months, P = 0.0458). At the final of follow up, the mean AOFAS score inautograft group was significantly increased compared with pre operation (62.3 ±8.2 vs. 95.1 ± 7.5, P = 0.0001), as well as the allograft group (60.2 ± 8.4 vs.94.8 ± 5.5, P = 0.0000). However, nosignificant difference in AOFAS was found between these two groups. There wasno significant different in talar tilt or shift between autograft and allograftgroups.
Conclusion:Reconstruction of the lateral ankle ligaments using a semitendinosus tendonautograft and a minimally invasive approach can result in a faster healing ofankle instability and not cause donor site morbidity.
Keyword:Lateralankle instability; Ligaments reconstruction; Semitendinosus autograft; Tendonallograft
INTRODUCTION
Acuteankle sprain isa common medical condition that the ligaments of the ankle are completely orpartially torn, accounting for 10·15 % of sports related injuries. Bridgman et al.has reported that thecrude incidence rate of ankle sprains rises from 52.7 per 10000 to60.9 in the UK, of which 14 % attending accident and emergency units areclassed as severe (i.e. 42000 severe ankle sprains per year).Although most of the patients have satisfactory functionrecovery after conservative treatments, some of themshow mechanical instability in the anterior talofibular ligament (ATFL), thecalcaneofibular ligament (CFL), and the posterior talofibular ligament (PTFL)and require operative intervention after several years.
Currently, there are multiple operative techniques for chronic ankleinstability, including anatomic repair (e.g. Broström, Karlssonmodified Broström, and Gould modifiedBroström), non anatomic reconstruction(e.g. Chrisman Snook and Evans procedures),and anatomic reconstruction. Anatomic repair involves the use of existingendogenous ligamentous tissues to restore the stability. If there are absent ofadequate soft tissues due to repetitive ankle sprains and surgeries,reconstruction may be preferable to repair. Non anatomic reconstructiontechniques stabilize the ankle using the peroneus brevis tendon, but do not reestablishthe anatomic ankle kinematics, possibly leading to ankle stiffness.Subsequently,scholars modify these techniques to create an anatomicreconstruction utilizing autograftor allografttendon.Studieshave demonstrated that anatomic reconstruction can not only significantly reduceboth lateral ankle instability and talar tilt, but also reestablish achievenormal kinematics.
The common autografttendons are mainly derived from extensortendon of the fourth toe, free plantaris and semitendinosus.Meanwhile, allografttendons mainly include anterior tibial tendon allograft and semitendinosustendon allograft.Previous studies have shown that there are no significantdifferences in short term clinical outcomes between allograft and autografttendon.Importantly, an allograft has the advantages ofno donor site morbidity, shorter operation time and less postoperative paincompared with the autograft. Thus, allograft tendon has become a more attractive option. However,a recent expected value decision analysis indicate patients' aversion toallograft tissue in general, and specific aversion to risk of diseasetransmission, resulting in a decision for autograft, independent of expectedoutcomes. Therefore, it is necessary to develop aminimally invasive surgery for autograft tendon to reduce the tendon donor sitemorbidity problems, which has been achieved in our previous study in2013. In present study, we aimed to further compare the clinical outcome ofanatomical reconstructions of the lateral ankle ligaments using semitendinosusautograft or tendon allograft (Osteorad Ltd, Shanxi, China) via a minimallyinvasive approach retrospectively.
MATERIALS AND METHODS
Clinical manifestation
From September 2006 toJune 2011, 68 patients sufferinglateral ankle instability were treated via anatomical reconstructionsof the lateral ligaments of the ankle in our hospital.These patients received the semitendinosus autograft (autograftgroup, 14 left /18 right) or tendon allograft (allograft group, 16 left /20right) according to their financial situation after we introduced theadvantages and disadvantages of both methods. The autograft group included 19males and 13 females with the average age of 32.4 ± 2.4 years, and theallograft group included 22 males and 14 females with the average age of 33.2 ±3.2 years. The average time of initial injury to surgery was 17.3 ± 2.1 monthsin the autograft group and 19.1 ± 4.9 months in the allograft group. In autograft group, 23 patients were followedwith average of 33.5 ± 6.7 months, while 26 patients were followed in allograftgroup with average of 28.5 ± 6.7 months (Table 1).
Table 1 Comparison of clinical manifestation ofpatients in autologous and allograft groups
Comparability | Autograft group | Allograft group group | P-value |
Clinical manifestation |
|
|
|
Gender (Male/Female) | 32(19/13) | 36(22/14) | 0.884 |
Average age (years) | 0.2525 | ||
Injured ankle (left/right) | 14/18 | 16/20 | 1.000 |
Body mass index | 30.5 ± 5.2 | 0.1178 | |
Time of initial injury to surgery (months) | 17.3 ± 2.1 | 19.1 ± 4.9 | 0.058 |
Operation outcome |
|
|
|
Operation time (min) | 85.5 ± 11.5 | 58.1 ± 10.2 | 0.0000 |
Duration of fever (days) | 2.5 ± 1.2 | 5.5 ± 1.5 | 0.0000 |
Time to heal (months) | 11.2 ± 4.1 | 13.5 ± 5.2 | 0.0458 |
Follow-up |
|
|
|
Patients | 23 | 26 |
|
Duration | 33.5 ± 6.7 | 28.5 ± 6.7 | 0.0122 |
Theindications for surgery were: (1) recurrentsprains more than twice within half a year; (2) severe ankle instabilityby a positive anterior drawer test (10 mm talar shift or 3 mm more than healthyside) or talar tilt (talar tilt > 9° or 3° more than healthyside); (3) failure of conservative treatments (rest, ice,compression, elevation, and support), Brostrom and Gould surgeries (5 patientsin autograft group and 7 patients in allograft group); and (4)obesity (body massindex > 25). All patients with the following surgery contraindications wereexcluded: (1) ankle infection; (2) fracture; and (3) ankle arthritis > grade 2according to Morrey and Wiedeman classification.
In addition, allpatients underwent weight bearing radiographs (anterior posterior,mortise, and lateral views) of foot, gait analysis, and signs collectionfor injuries of ATFL, CFL and PTFL, such as swelling, congestion and tendernesspreoperatively.
Surgical operation
Anarthroscopic·assisted minimally invasive surgery was performed on all patients asdescribed in our previous study. After general or continual epiduralanesthesia, the patients were supinely placed and the knee of affected limb wasbended and rotated laterally. A tourniquet was routinely applied at the proximalthigh.
Afterperforming a diagnostic arthroscopy verifyingankle instability (Figure 1), the semitendinosustendon was harvested from theipsilateral affected limb via a two-incision technique (Figure 2) in which the proximalincision was made at the most medial tendon 2 cm above the jointline and the distal incision was made 2 cm medial to thetibial tuberosity. After the 2 ends of the tendon were exposed, the semitendinosustendon was isolated using a specialized tendon stripper, released from thedistal end, extracted from the proximal incision, and finally immersed inphysiological saline until use after being woven withthe 20 absorbable muscle tendon suture (Johnson & Johnson Medical Ltd.Sommerville NJ, USA).
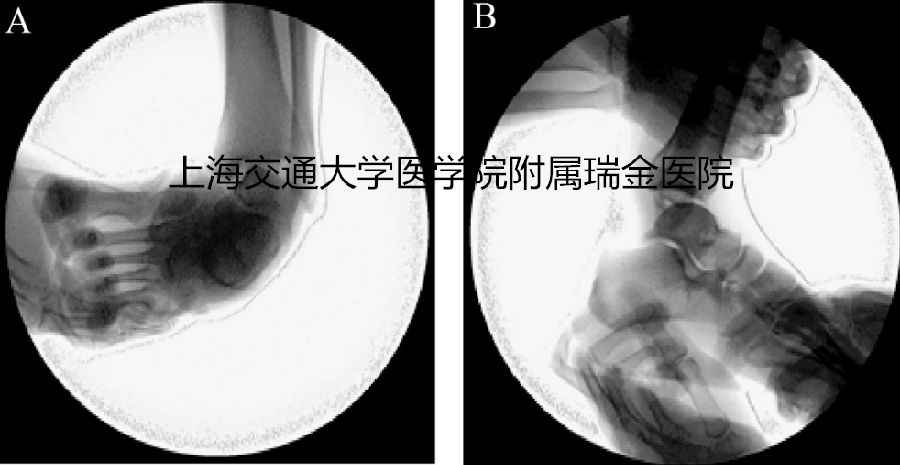
Figure 1 The C-armfluoroscopic examination of lateral ankle instability. A and B represented anterior-posteriorand lateral views.
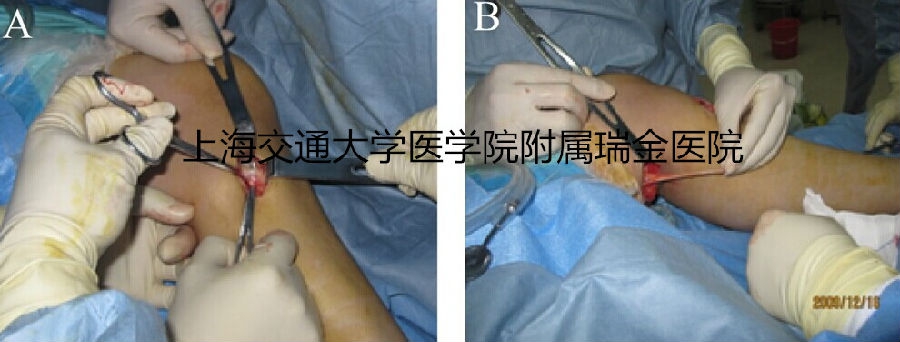
Figure 2 Thesemitendinosus tendon autograft was harvested with a minimally invasivetechnique.
A.Distal end of semitendinosus tendon. B. Proximal end of semitendinosus tendon.
Theallograft ligamentpurchased from Osteorad Ltd (Shanxi, China) was trimmed to 14 cm (in length) × 8 mm(in width) × 1 mm (in thickness) after cryogenic processing and thenwoven through the 2-0 absorbable muscle-tendon suture (Johnson & JohnsonMedical Ltd. Sommerville NJ, USA).
At the recipient siteof the ankle, 4 small incisions (5 mm in diameter) were madeat the medial and lateral side of the fibular tip, the talar neck, and themiddle portion of the calcaneus (Figure 3). Two guide wires were introducedtransversely at the distal end of the fibula. Two holes were then drilled overthe guide wire from each end to form a tunnel (4.5 mm in diameter, incline of 120°). Theprepared semitendinosus tendon autograft was introduced through the tunnel by along eyelet needle. The ends of the tendon were then passed above the bonesurface to the incisions at the talar neck and calcaneus. Guide wires wereplaced for positioning of talar and calcaneal tunnels under Carm fluoroscopy.A 7 mm × 23 mm biodegradableinference screw (polylllactic acid, BioCryl®, DePuyMitek) was used to fix the tendon graft in the talarneck and calcaneus. The location of interference screws was also detected underC-armfluoroscopy.
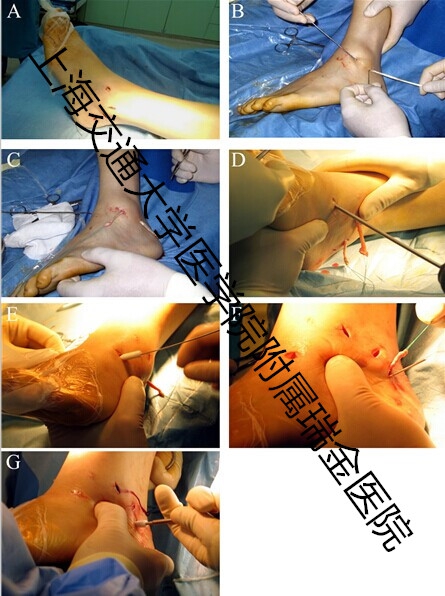
Figure 3 Anatomicalanterior talofibular ligament (ATFL) and calcaneofibular ligamentreconstruction by semitendinosus tendon autograft with a minimally invasivetechnique.
A. 4 small incisions (5 mm) at the lateral malleolus.B. Tendon loaded on eyelet needle for passage of the graft traction suture andtendon through distal fibula. C. Tendon with traction suture at both ends.Middle part of tendon is inside distal fibular tunnel. D. Clamp 2 guides clamp1 through the subcutaneous tunnel. Then clamp 1 holds traction suture and leadstendon through tunnel to talar neck. E. Interference screw was used to fix oneend of tendon to the talus to reconstruct ATFL. F. The other end of tendon wasintroduced into body of calcaneus. G. The foot was slightly everted whileinserting the interference screw into the calcaneus to keep the tension onlateral ligament.
Postoperative management
After operation, smokingof patients and surrounding people was prohibited. The affected foot wasimmobilized in a valgus position and a weight free manner using aUshaped plaster. Antibiotics were routinely used within 24 h after operation.Isometric strength exercise of the extension of the ankle was allowed to reducestiffness at 3 days after operation. Four weeks after the surgery,the plaster was changed to an ankle orthosis and partial weight·bearingexercises were encouraged. Six weeks after the surgery, full weight bearingexercises were permitted. The ankle orthosis was removed at 10 weeks afteroperation and walking with a softbrace (Company OPED, Valley, Germany) forexercises was allowed. The joggingwas resumed at 12 weeks after operation.
Evaluation oftherapeutic efficiency
The operative data between 2 groups wererecorded and analyzed, including operation time (min), duration of fever(>37°C, days) and time to heal (can walk on unevenground steadily, months). The outcome of surgical treatment was evaluated usingthe clinical rating scale of American Orthopaedic Foot and Ankle Society (AOFAS,100 points total). This scoring system classified the evaluated items intothree major categories: pain, function and alignment. In this scale, 50 pointswere assigned to function, 40 points to pain, and ten points to alignment.Usually, a score between 90 and 100 is excellent, 80·89 good, 70·79 fair and< 70 poor . Donor site morbidity was assessed by subjective sensation of thedonor site area, range of motion of the knee and strength. Postoperative stressradiographs were taken using a TELOS stress device (TELOS, METAX, Germany) at150 N.
Statistical analysis
Statistical analysiswas performed using SPSS13.0 software (Chicago, IL, USA). The wilcox and signdedtests were used for statistical analysis of pre- and post-operative AOFAS. Thesignificance level was defined as P < 0.05.
RESULTS
The average operation time wassignificantly increased in autograft group compared with allograft group (85.5± 11.5 min vs. 58.1 ± 10.2 min, P = 0.0000). However, the fever days and timeto heal were significantly longer in allograft group (5.5 ± 1.5 days vs. 2.5 ±1.2 days, P = 0.0000; 13.5 ± 5.2 months vs. 11.2 ± 4.1 months, P =0.0458) (Table 1).
At the final of follow up, the meanAOFAS score in autograftgroup wassignificantly increased compared with pre operation (62.3 ± 8.2 vs. 95.1 ± 7.5,P = 0.0000), as well as the allograftgroup (60.2 ± 8.4 vs. 94.8 ± 5.5, P = 0.0000) (Table 2). However, no significantdifference in the AOFAS wasfound between two groups preoperatively and at the final of follow up. Thesatisfaction level was excellent in 16 patients and good 5 patients inautograft group, while excellent in 17 patients and good in 6 patients inallograft group. Three patients of autograft group and 2 of allograft groupwalked unsteadily on the uneven ground. One patient of autograft group walkedunsteadily in daily life. No patients complained of weakness or disability inthe donor site.
Table 2 The AOFAS score, talar tilt and talarshift of pre-operation and final follow-up.
| Autograft group | Allograft group | P-value* |
AOFAS score (point) |
|
|
|
Preoperatively | 62.3 ± 8.2 | 60.2 ± 8.4 | 0.0000 |
Final follow-up | 95.1 ± 7.5 | 94.8 ± 5.5 | 0.0000 |
Talar tilt (°) |
|
|
|
Preoperatively | 14.0 ± 3.2 | 13.0 ± 3.5 | 0.0000 |
Final follow-up | 3.8 ± 1.2 | 3.6 ± 1.4 | 0.0000 |
Talar shift |
|
|
|
Preoperatively | 12.3 ± 3.2 | 11.5 ± 2.3 | 0.0000 |
Final follow-up | 4.6 ± 1.2 | 4.3 ± 1.5 |
*compared with preoperatively
Compared with pre·operation, theanterior drawer stress showed reduced talar tilt (from 14.0 ± 3.2° to 3.8 ± 1.2°)and talar shift (12.3 ± 3.2 mm to 4.6 ± 1.2 mm) at the final of follow up inautograft group, as well as allograft group (talar tilt from 13.0 ± 3.5° to 3.6 ± 1.4°, talar shiftfrom 11.5± 2.3 mm to 4.3 ± 1.5 mm) (Table 2). There was nosignificant difference in talar tilt or talar shift between autograft andallograft groups.
Although the longer fever days and time to healneeded in allograft group, no evidence of sterile effusion overlying theabsorbable screws was detected. Nine patients with postoperative swelling weretreated via dressing change, oral use of indomethacin or dexamethasone therapy.After 5·7 days, the swelling had gone down and wound had been properly healed.
DISCUSSION
Although severalstudies have demonstrated no significant differences in clinical outcomesbetween allograft and autografttendon for reconstruction ofthe lateral ankle ligaments, allograft reconstruction is significantly moreexpensive than autograft reconstruction and has potential for diseasetransmission, limiting its acceptance for routine ankle reconstruction.Therefore, autograft tendon is still preferable for most patients. To reducethe disadvantages of autograft tendon (donor sitemorbidity), in 2013, we performed a minimally invasive approach forreconstruction of lateral ligaments of the ankle using semitendinosusautograft. The semitendinosus tendon is relatively easy to harvest and it islarger in diameter and provides a stronger graft for simultaneousreconstruction of the ATFL and CFL. Previous studies has demonstrated minimaldonor site morbidity was developed using semitendinosus tendon. As expected,our results showed that no patients complained of weakness or disability in thedonor site. In consistent with previous literatures, our clinical results alsoshowed no significantdifferences in the improvement of AOFAS, talar tilt, and talar shift between autograftand allograft groups.
In addition, because additional time wasrequired for autograft graft preparation, the average operationtime was significantlyincreased in autograft group compared withallograft group (85.5 ± 11.5 min vs. 58.1 ± 10.2 min, P = 0.0000). Thus, somescholars believe that the cost of the allograft itself appears to be offset bythe increased operating room time and a greater likelihood of overnighthospitalization for autograft procedures. However, a recent expected·valuedecision analysis indicates patients' aversion to allograft tissue in general. Thismay be attributed to longer fever days and time to heal in allograft group (5.5± 1.5 days vs. 2.5 ± 1.2 days, P = 0.0000; 11.2 ± 4.1 months vs. 13.5 ± 5.2 months,P = 0.0458). The reason of long time fever is associated with the host immuneresponse to allograft, heat of absorption and the real ability of tissue banksin our country to process allografts. The different collagen content andmechanical strength of the allograft tendon from the native ankle ligamentscontributes to the more time to heal, which may influence patients’ quality oflife and quick back to work. Yamazaki et al. reported that an increase thelength of the bone tunnel was positively correlated with the quality andstrength of the reconstruction. Minimizing the mismatch of diameters between graftand tunnel may tighten the fit of the graft in the tunnel and improves healing.In this study, a 4.5 mm drill was used to create a tunnel that can be widenedto 7 mm with an approximate depth of 23 mm. A 7 mm × 23 mm biodegradableinference screw was used to fix the tendon graft in the talar neck andcalcaneus. Thus, the time to heal was shorter in autograft group and no majorpostoperative complications (talar neck fractures, osteolysis or steriledrainage) occurred.
This study had several limitations. The first wasthe retrospective nature of the study. This may be the reason to the differentfollow up time in two groups. Secondly, the follow-up time of bothgroups is relatively short, long term follow-up should be done to furtherevaluate their clinical outcomes. Thirdly, the sample size is small.
In conclusion, we retrospectively analyzed theeffectiveness of semitendinosus autograft and tendon allograft used foranatomic reconstruction of ligaments of chronic ankle instability. Combined onthe minimally invasive surgery with small incision, the healing ofsemitendinosus autograft was slightly faster than the tendon allograft and nodonor site morbidity was observed. The clinical outcomes of the two grafts wereboth excellent and no significant difference was identified. However, furthermulti-centric study is still needed with larger sample size and longer followup.
参考文献(略)
上海交通大学医学院附属瑞金医院 徐向阳 胡牧


 京公网安备11010502051256号
京公网安备11010502051256号