Retrospective study on posterior malleolus fracture
2014-12-04 文章来源:北京大学人民医院 姜保国 我要说
骨科在线版权所有,如需转载请注明来自本网站.
Purpose:This retrospective study evaluated the treatmenteffect of ankle joint fracturesurgery involving the posterior malleolus anddiscussed relevant factors influencing the occurrence oftraumatic arthritis of the ankle joint.
Methods:A total of 102 cases of anklejoint fracture involving the posterior malleolus infive large scale skeletal trauma centres in China from January 2000 to July2009 were retrospectively analysed in terms of surgical treatment and completefollow up.Ankle joint mobility, posterior malleolus fragment size, articularsurface evenness, Ankle Hindfoot Scale of the AmericanOrthopedic Foot and Ankle Society (AOFAS) score, and imaging scale score forarthritis were recorded. The degree of fracture painduring rest, active movement, and weight bearing walking and satisfaction withtreatment were evaluated using a visual analogue scale (VAS).
Results: The average AOFAS score was 95.9, excellence rate was 92.2%, andaverage VAS scores for degree of fracture pain during rest, active movement,and weight bearing walking were 0.15, 0.31, and 0.68. Thirty six cases showed arthritis manifestations. Ankle joint mobility along alldirections on the injured side was lower than that on the unaffected side.There was no obvious difference in treatment effect between the fixed andunfixed posterior malleolus fragment groups for all and for fragment size of<25% and between fixing the posterior malleolus fragmentfrom front to back or from back to front and between elderly patients (≥60years old) and young patients (<60 years old). There was distinct differencein treatment effect between articular surface evenness and unevenness for alland for fragment size of ≥25%.
Conclusions:For all 102 cases of ankle joint fracture involvingthe posterior malleolus, the treatment effect was satisfactory. Restoration ofan even articular surface especially when fragment size ≥25% should beattempted during treatment.
Keywords:posterior malleolus fracture, articular surfaceevenness, traumatic arthritis, retrospective study
Introduction
Ankle joint fracture is clinically common and accounts for 3.92% of all fractures sustained in the entire body. Approximately 7% to 44% of ankle joint fracturesare accompanied by posterior malleolus fracture, whichis rarely seen alone. Ankle joint fracture canreportedly easily cause traumatic arthritis if it involves the posteriormalleolus, and the fracture prognosis is poor. Somescholars have suggested that arthritis is triggered bychange in the stress distribution on the articularsurface, which is caused by change in the articular surface area at thedistal end of the tibia after posterior malleolusfracture. The indications for fixation of posteriormalleolus fragments are controversial. Most scholars consider that the posterior malleolus fragment should be fixed when it accounts for ≥25% of the articular surface at the distal end of the tibia .Langenhuijsen et al. believe that the posteriormalleolus fragment should be fixed surgically when the fragment is ≥10% and thearticular surface at the distal end of the tibia is still uneven after incision fixation of the medial and lateral malleolus.However, reported cases are few and dependability of results needs furtherverification.
This multicentre retrospective study evaluated the treatment effect ofankle joint fracture involving the posterior malleolus, analysed the impact ofdifferent posterior malleolus fragment sizes on thetreatment effect (respectively taking 25% and 10% as the dividing lines), andstudied the impact of screw direction during posteriormalleolus fragment fixation and articular surface evenness after reductionon prognosis. The influencing factors causing traumatic arthritis duringposterior malleolus fracture are also herein discussed.
Materialsand methods
Patients and inclusion criteria
Patients with ankle joint fractures treated atskeletal trauma centres of five large scale hospitals (People’s Hospital of Peking University, Jishuitan Hospital of PekingUniversity, Xuanwu Hospital of Capital Medical University, West China Hospitalof Sichuan University, and South Hospital of Southern Medical University) fromJanuary 2000 to July 2009 were evaluated.
The inclusion criteria were patients (1) with a definitivediagnosis of ankle joint fracture based on clinical and imagingtechnologies, (2) undergoing open reduction internal fixation surgery, (3) withinvolvement of the posterior malleolus, and (4) with complete clinicalfollow-up data.
Study method
Datacollection
All workers participating in this study receivedunified training to fully understand the purpose andspecific process of the study. All workers visited patients postoperativelyaccording to a unified ankle joint fracture surgery treatment follow up form.The follow up activity included acquisition of outpatient follow upinformation. All follow up results were input into a database, 102 cases ofankle joint fracture involving the posterior malleolus with complete follow-upinformation were selected, and further analysis was performed.
Measurementand evaluation indices
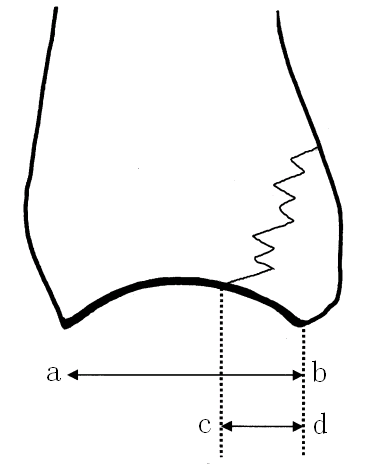
The posterior malleolusfragment size was calculated as the percentage of theinvolved distal tibial articular surface. The proportion ofthearticular surface of the fragment compared with the entire articularsurface at the distal end of the tibia was measured on the lateral X ray of theankle joint (see Figure 1). The articular surface waschecked for evenness after reduction of the posterior malleolus fragment. Thesurface was determined to be even at a level of ≤1 mm and uneven at a level of >1 mm.
The arthritis imaging score according to X ray films of the ankle jointtaken during the postoperative follow up was recorded: 0 indicated a normaljoint, 1 indicated osteophytes but no joint space narrowing, 2 indicated joint space narrowingwith or without osteophytes, and 3 indicated disappearance or deformation ofthe joint space.
The evaluation indices also included the Ankle-Hindfoot Scale of theAmerican Orthopedic Foot and Ankle Society (AOFAS scale)score (excellent, ≥90; good, 75–89; acceptable, 50-74; poor, <50); fracturepain during rest, active movement, and weight bearing walking based on a visualanalogue scale (VAS) (0, painfree; 10, the most unbearable pain); and anklejoint mobility (angle of dorsiflexion, plantarflexion, varus, and valgus during follow-up).
Statisticalmethods
Statistical analysis was conducted with SPSS 15.0 for Windows softwareand included the paired t test, nonparametricMann Whitney test, Kruskal Wallis test. A p valueof <0.05 represented a statistically significant difference.
Results
General data
This study included 41 males and 61 females with a mean age of 43.4(15-80) years. Causes of injuries included 13 cases of traffic injury, 36 casesof sprain, 50 cases of fall down injury, nine cases of crush injury, and onecase of falling injury.The fractures were divided into different typesaccording to the Arbeitsgemeinschaft für Osteosynthesefragen/Orthopaedic TraumaAssociation (AO/OTA) fracture classification system: there were two cases oftype A (2%), 78 cases of type B (76%), and 22 cases of type C (22%). Theaverage posterior malleolus fragment size was 19.1%. Sixteen cases (6.3%) had afragment size of <10%, 24 cases (34.7%) had a fragment size of ≥25%, and 62cases (16.3%) had a fragment size of 10% to 25%. The posterior malleolusfragment was surgically fixed in 42 cases (41.2%). The articular surface afterreduction of the posterior malleolus fragment was even in 78 cases (76.5%) anduneven in 24 cases (23.5%).
Treatment effect
The follow up periodwas 6.9 to 102.3 months (average, 33.8 months), and clinical union of thefracture was achieved in all patients. The AOFAS score was 95.9±5.7 andincluded 70 excellent cases (68.6%), 24 good cases (23.6%), and eight acceptablecases (7.8%); the excellence rate was 92.2%. The average VAS score for fracturepain under different conditions was 0.15±0.56 during rest, 0.31±0.90 duringactive movement, and 0.68±1.47 during weight bearing walking. There werestatistically significant difference in the VAS scores under these threeconditions (χ2=32.125, p<0.01).However, the average of the three groups was <1, indicating only slightpain. The average satisfaction with treatment was 9.62±0.56 (7 10). Thirty sixcases (35.2%) showed arthritis manifestations according to imaging results,including 31 cases (86.1%) with a score of 1, 5 cases (14.9%) with a score of2. For cases with or without arthritis manifestations, the VAS fracture painscore under different conditions showed no statistical differences (p>0.05).
Statistical analysis
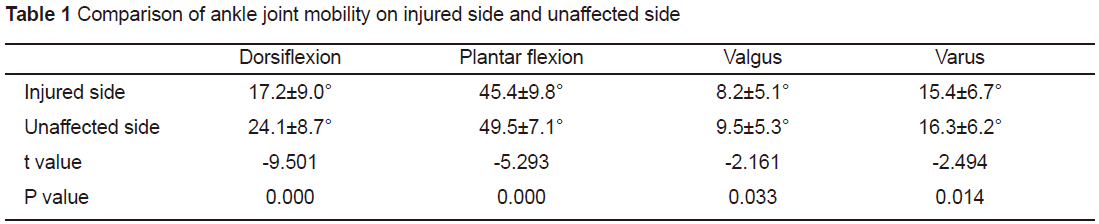
Ankle joint mobilitywas compared between the injured and unaffected sides. The paired t testresults showed significant differences in ankle joint mobility along alldirections between the injured and unaffected sides (p<0.05). (see Table 1).
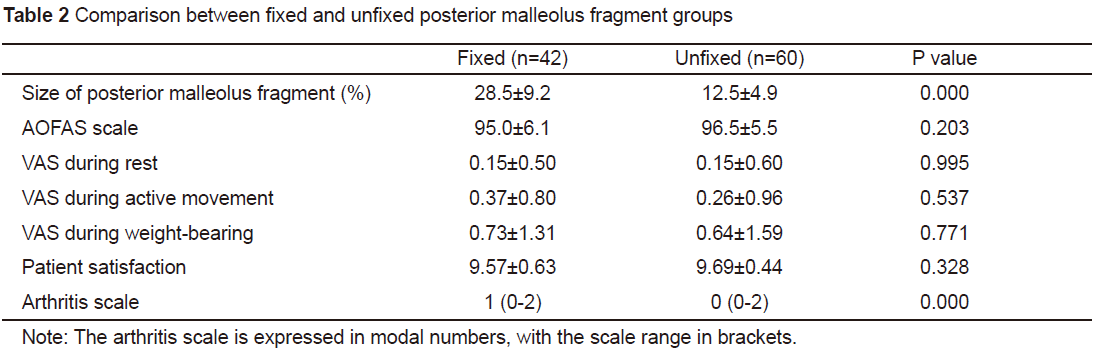
Comparisonwas also performed between the fixed and unfixed posterior malleolus fragmentgroups. The fixed group comprised 42 cases with an average fragment size of28.5% (11.1%-55.0%); the unfixed group comprised 60 cases with an averagefragment size of 12.5% (1.5%-24.3%). The posterior malleolus fragment size andarthritis score of the two groups showed statistically significant differences,while the difference in the AOFAS score, VAS rating under various conditions,and patient satisfaction rating showed no statistically significant differences(see Table 2). The average surgically fixed posterior malleolus fragment sizewas larger than the average unfixed posterior malleolus fragment size, whichindicates that the larger the posterior malleolus fragment, the greater thepotential for successful surgical fixation. Comparison of the AOFAS score, VASrating, and patient satisfaction showed that there was no statisticaldifference in the treatment effect between the fixed and unfixed posteriormalleolus fragment groups. The difference in the arthritis score may have beenrelated to the posterior malleolus fragment size, which was furtherstatistically analysed (below). In the fixed and unfixed posterior malleolusgroups, the articular surface after fracture reduction was even in 27 and 49cases, respectively. Comparison showed that the difference was statisticallysignificant (p=0.047); i.e., the evenarticular surface accounted for a higher number of cases in the unfixed group.In the fixed group, a large posterior malleolus fragment, serious injury, anddifficult reduction of the articular surface may have caused the low proportionof even articular surfaces.
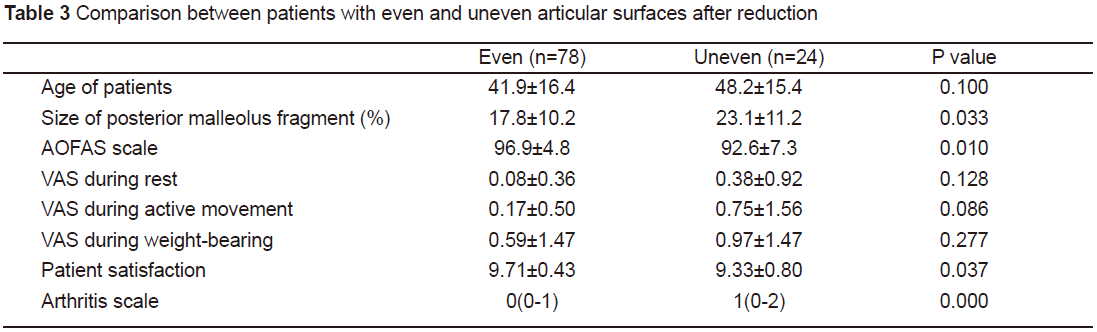
Allposterior malleolus fracture cases were divided into two groups according toarticular surface evenness after reduction to compare the posterior malleolusfragment size, AOFAS score, VAS score, patient satisfaction, and arthritisscore of the two groups. Distinct differences were shown in the posteriormalleolus fragment size, AOFAS score, arthritis score, and patientsatisfaction, while there was no statistical difference in the VAS score underthe three conditions (see Table 3). These results indicate that the articularsurface reduction level affects the prognosis of the posterior malleolusfracture and that the posterior malleolus fragment size influences articularsurface evenness.
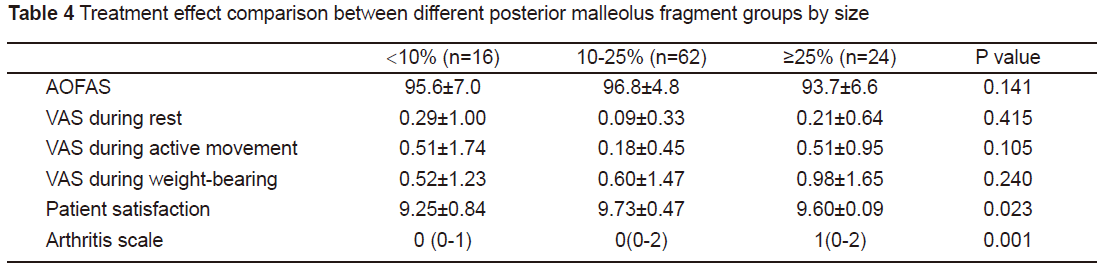
Allcases were divided into three groups (<10%,10%-25%, and ≥25%) by taking 10%and 25% (posterior malleolus fragment size) as the dividing lines to comparethe treatment effect among the three groups. There were no statisticaldifferences in the AOFAS and VAS scores under various conditions, while therewere statistically significant differences in patient satisfaction andarthritis score (see Table 4). Patient satisfaction was lowest when fragmentswere <10% and highest when 10% to 25%. The average patient satisfactionvalue was >9 in allgroups, indicating that the overall treatment effect was satisfactory. Thearthritis score for different posterior malleolus fragment sizes differedgreatly, indicating that the posttraumatic arthritis may be related to thefragment size.
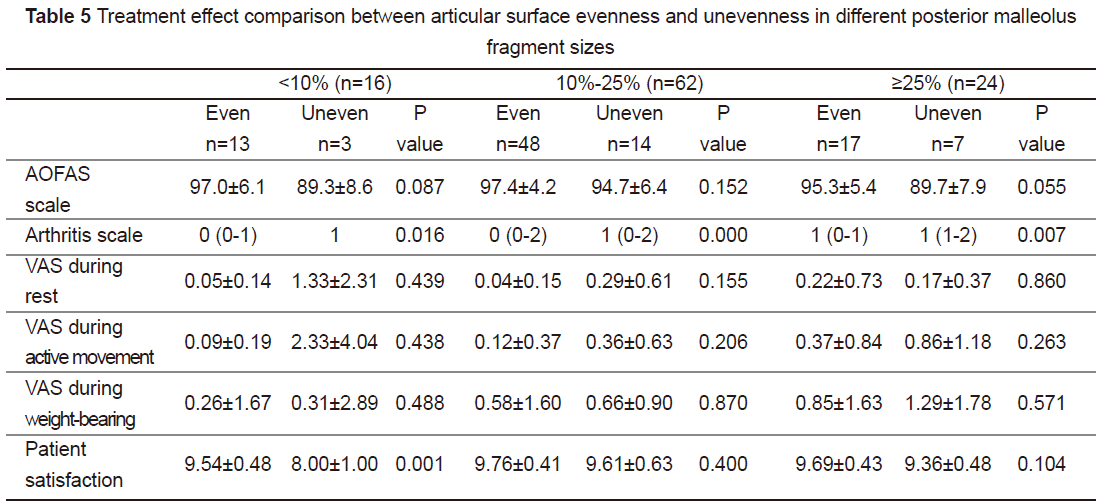
We respectively analysed the relationship betweenarticular surface evenness after fracture reduction and prognosis among thethree above described posterior malleolus fragment groups (<10%, 10%-25%,and ≥25%) (see Table 5). The AOFAS and VAS scores in the three groups showed nosignificant differences. Comparison of the arthritis score showed that thisindex was significantly different among the various fragment groups. Patientsatisfaction differed greatly only in the group with a fragment size of<10%, but the reliability of statistical results was not high because of thesmall sample number in this group. According to the average value of thedifferent evaluation indices in these groups, for patients with even articularsurfaces, AOFAS score and patient satisfaction were higher, while VAS score forfracture pain under different conditions was lower than that of patients withuneven articular surfaces.
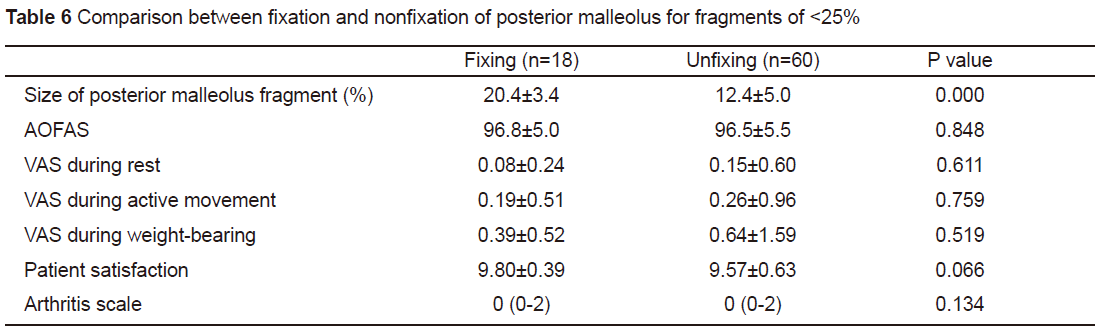
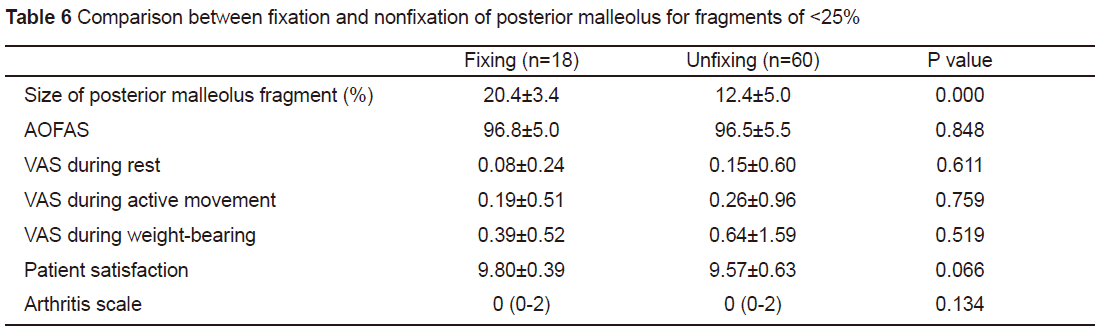
For a posterior malleolus fragment size of<25%, the malleolus fracture was fixed in 18 cases and unfixed in 60 cases.Comparison of the treatment effect in the two groups shows a statisticalsignificant difference in the posterior malleolus fragment size, while therewere no statistical differences in the AOFAS score, VAS score, patientsatisfaction, and arthritis score (see Table 6). This shows that amongfragments of <25%, larger fragments are inclined to fixation, but whetherfixation occurs does not affect the treatment effect.
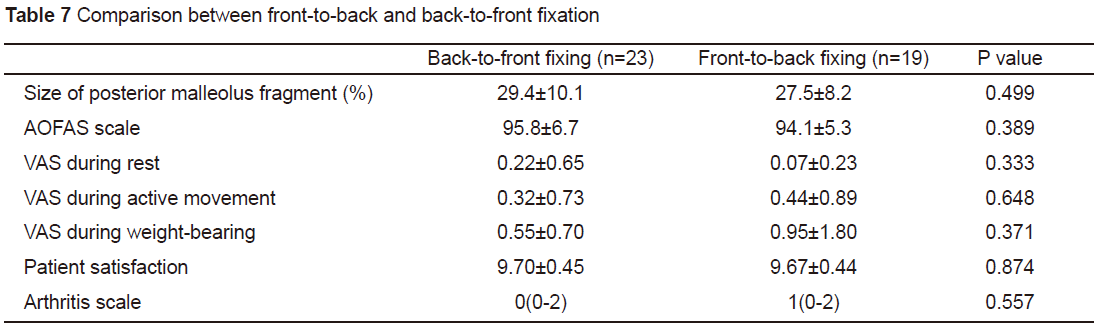
Among 42 cases involving fixation of the posteriormalleolus fragment, 23 underwent back to front fixation with an averagefragment size of 29.4% (14.8%-55.0%); the remaining 19 cases underwentfront to back fixation with an average fragment size of 27.5% (11.1%-45.4%).The impact of different fixation directions on the treatment effect wasstatistically analysed. The results showed no obvious difference (see Table 7),which indicates that fixation direction of the posterior malleolus fragmentexerts no impact on the treatment effect. In the front to back fixation group,the articular surface was even in 13 cases and uneven in six cases; in theback to front fixation group, the articular surface was even in 15 cases anduneven in eight cases. No statistical significant difference was found aftercomparison of the two groups (χ2=0.048, p>0.05).
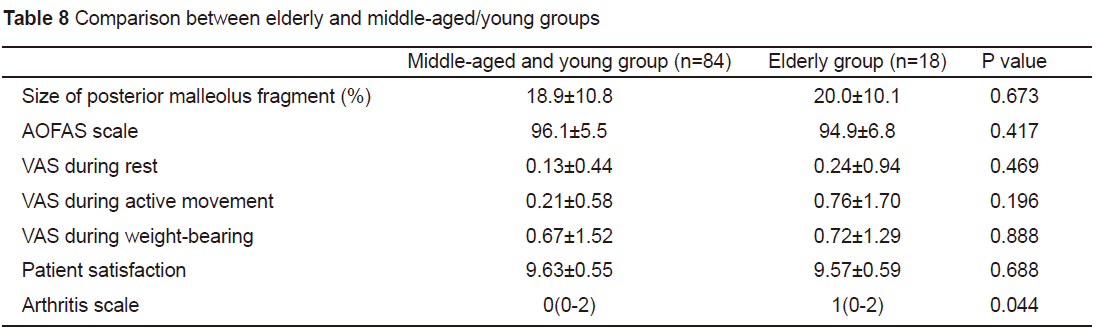
The treatment effect between elderly and youngpatients was compared. We divided the cases into two groups: the elderly group(≥60 years of age, n=18) and middleaged/young group (<60 years of age,n=84). The posterior malleolus fragment size, AOFAS score, VAS score, patientsatisfaction, and arthritis score were analysed. There was no statistical differencein the above indices with the exception of the arthritis score (see Table 8).This indicates that the treatment effect between elderly and middle-aged/youngpatients was basically the same, but the arthritis score in elderly patientswas higher than that in middle-aged/young patients.
Discussion
This study showed that ankle joint mobilityalong all directions on the injured side was lower than that on the unaffectedside, indicating that posterior malleolus fracture can greatly affect ankle jointmobility. However, from the perspective of overall treatment effect, theaverage AOFAS score was 95.9; the excellence rate was 92.2%; and the averageVAS score for fracture position during rest, active movement, andweight bearing walking was 0.15, 0.31, and 0.68, respectively, which are higherthan those reported by other studies. Average patient satisfaction withtreatment reached a score of 9.62, demonstrating that the treatment effect inthis group was satisfactory.
Comparisonof the fixed and unfixed posterior malleolus groups showed that the posteriormalleolus fragment in the fixed group was significantly larger than that in theunfixed group. The arthritis score also differed greatly, but the AOFAS and VASscores did not show obvious statistical differences. De Vries and Langenhuijsenet al. also reported that fragment sizes differ greatly, but there were nostatistical differences in functional and VAS scores between fixed and unfixedposterior malleolus fragments. However, these papers evaluated few posteriormalleolus fixation cases (11–14 cases), so the results reliability is low.
Weanalysed the relationship between articular surface evenness and prognosis ofposterior malleolus fracture. The results showed that an even articular surfaceis accompanied by a smaller fragment and that its AOFAS score, patient satisfaction,and arthritis score are better than those of an uneven articular surface. Thisindicates that the posterior malleolus fragment size is related to theachievement of anatomical reduction of the articular surface. The larger theposterior malleolus fragment, the more damaging the force. Thus, the difficultyof achieving articular surface reduction is increased.
Wedivided the fragments into three groups (<10%, 10%-25%,and ≥25%) by taking10% and 25% as the dividing lines. After statistical analysis of the treatmenteffect among the three groups, we found great differences in patientsatisfaction and arthritis score. Arthritis was most serious when the fragmentwas ≥25%, while satisfaction was highest when the fragment size was 10% to 25%.However, the average score of all three groups was >9. Lindsjo, and Broosand Bisschop stated that the treatment effect is poor for patients with largefragments. De Vries did not find a relationship between fragment size andlong term prognosis. He believes that this may have been due to an insufficientsample size. We further analysed the relationship between articular surfaceevenness and prognosis with various fragment sizes. Among the three groups, thearthritis score in patients with uneven articular surfaces was higher than thatin patients with even articular surfaces. In the group with fragments of<10%, satisfaction of patients with even articular surfaces was higher thanthat of patients with uneven articular surfaces. In the other fragment groups,there was no obvious correlation between articular surface evenness andprognosis. However, according to the average values, the treatment effect inpatients with even articular surfaces was better in all groups. This reminds usto attempt anatomical reduction of the posterior malleolus fragment to reducesubsequent traumatic arthritis risk. When the posterior malleolus fragment is≥25%, arthritis severity exceeds that of fragments of <25% regardless of thesurgical fixation effect. Analysis of all cases showed that articular surfaceevenness was related to prognosis, but the relationship was not obvious amongdifferent fragment sizes. One possibility is that the decreased number ofsamples after grouping caused deviation in the results.
There are always disputes on the indication for posterior malleolusfragment fixation. Raasch et al. and Fitzpatrick et al. considered thatposterior malleolus fractures can be stably reduced under general conditionswithout fixation as long as the medial and lateral malleolus are intact or thefracture position is firmly fixed; posterior malleolus fractures with poorreduction during the first phase may subsequently undergo a natural reductionprocess if they are not fixed; the natural correction opportunity is lost iffixation is performed in poorer positions. Papachristou found that ankle jointstress is mainly concentrated in the two middle quarters of the articularsurface area, while the rear quarter of the articular surface hardly bears aload. Posterior malleolus fixation is performed in all cases with fragments of≥25%, so we cannot compare the treatment effect of fixed and unfixed fragmentsof ≥25%. However, for fragments of <25%, we compared the treatment effectwith and without fixation. Fixation of the posterior malleolus fragment did notgreatly affect the treatment effect. However, such a result based on aretrospective study is not adequate to indicate that no fixation is requiredwhen the fragment is <25% and only provides a reference value. Lack of clearbiomechanical proof and universal standard quantification indices forevaluation of the ankle joint fracture treatment effect is another reason forunclear posterior malleolus fixation indications.
Thereare also disputes on the posterior malleolus fixation mode, includingfront to back and back to front fixation. Both have advantages anddisadvantages. The former is simple in operation and convenient in removal, butit is difficult to reach firm pressurisation. While the latter has a soundpressurisation effect, the operation and removal during the second phase aredifficult. We statistically analysed the two fixation modes. There were nostatistical differences in the AOFAS, VAS, arthritis, and patient satisfactionscores under the two modes, which reminds us to ensure a satisfactory effect byusing front to back fixation. Mingo Robinet et al. reported 45 cases ofposterior malleolus fracture, including 18 cases involving posterior malleolusfixation. Among 15 cases of front to back fixation, fragment reduction was affectedin six because the screw thread appeared in the fracture line. Three cases ofback to front fixation achieved anatomical reduction. We also noticed thisproblem during treatment; the thread must penetrate the rear cortex of theposterior malleolus when conducting front to back fixation. Back to frontfixation should be adopted if the fracture bone is small enough to achieve goodpressurisation. In this study, the proportion of articular surface evennessunder different directions showed no statistical difference between the two.
In this study, 36 cases showed traumatic arthritis manifestations basedon imaging, accounting for 35.2% of all cases. When we compared the treatmenteffect in different posterior malleolus fracture groups, the arthritis scorealways showed statistically significant difference, but a hybrid effect oftenexisted between various factors. Comparison of the treatment effect withdifferent articular surface evenness showed that AOFAS score and patientsatisfaction with treatment in patients with an even articular surface weresignificantly higher than those in patients with an uneven articular surface.This reminds us to pay more attention to the reduction quality of the posteriormalleolus fragment when treating posterior malleolus fracture to acquire aneven articular surface after reduction.
Interms of measurement of the posterior malleolus fragment size, Langenhuijse,Mingo Robinet, other authors, and we adopted the proportion of linear distancebetween two points on the articular surface and the fracture line. However,this method may not be accurate because the posterior malleolus fracture lineis not often perfectly perpendicular to the lateral X ray plane, which resultsin overestimation or underestimation of the posterior malleolus fragment size.Ferries et al. pointed out that the credibility for determining fragment sizeby common plane films is low, and the error rate is very high, even forexperienced inspectors. Moreover, the articular surface at the distal end ofthe tibia is a curve surface rather than a flat surface; thus, estimation offragment size using only the proportion of the distance between the two pointscan also cause error. Magid et al. and Haraguchi et al.proposed that thecalculation method for fragment size based on CT images is more accurate.
Conclusion
For all 102 cases of ankle joint fractureinvolving the posterior malleolus, the treatment effect was satisfactory. Afterreduction of the posterior malleolus fragment, articular surface evenness atthe distal end of the tibia will affect the treatment effect of posteriormalleolus fracture; therefore, we should attempt to restore an even articularsurface especially when fragment size ≥25% during treatment.
Conflictof Interest
The authors declare that they have no conflictof interest.
参考文献(略)


 京公网安备11010502051256号
京公网安备11010502051256号