Medial Displacement Calcaneal Osteotomy with Posterior Tibial Tendon Reconstruction for the Flexible Flatfoot with Symptomatic Accessory Navicular
2015-01-04 文章来源:重庆西南医院 唐康来 我要说
abstract We investigated theclinical outcomes after medial displacement calcaneal osteotomy withreconstruction of the posterior tibial tendon insertion on the navicular, inpatients with flexible flatfoot with accessory navicular symptoms. FromDecember 2008 to July 2011, 16 patients (21 feet) with a flexible flatfoot,symptomatic accessory navicular, and obvious heel valgus underwent medialdisplacement calcaneal osteotomy and reconstruction with posterior tibialtendon insertion on the navicular bone. The patients were evaluated preoperatively,6 weeks and 3, 6, and 12 months postoperatively, and every 6 months thereafter.The clinical examination was undertaken using the American Orthopaedic Foot andAnkle Society ankle and midfoot scores. The radiologic assessments included thearch height, calcaneus inclination angle, talocalcaneal angle,and talar firstmetatarsal angle on the lateral weightbearing radiograph. The talocalcanealangle and talar first metatarsal angle was assessed on the anteroposterior viewof the weightbearing foot. Heel valgus alignment was assessed on the axialhindfoot radiographs. The mean follow·up duration was 28.5 months (range 18 to 48).All patients were satisfied with the clinical results and were pain free 6months postoperatively. No cases of wound infection or nerve injury developed.The mean American Orthopaedic Foot and Ankle Society score improved from 53.3± 6.5 to 90.8 ±1.4 at the last follow·upvisit (p < .01). The improvements in all radiographic parameters werestatistically significant between the preoperative and last follow·up examinations(p < .01). The heel valgus of all patients was corrected. Our results haveshown that medial displacement calcaneal osteotomy with reconstruction of theposterior tibial tendon insertion on the navicular bone is an effectivetreatment of flexible flatfoot with symptomatic accessory navicular, associatedwith excellent clinical outcomes and correction of the deformity. 2014 by theAmerican College of Foot and Ankle Surgeons. All rights reserved.
Flatfoot deformity in adults is mostly caused by posterior tibial tendondysfunction. Johnson and Strom, and later, Myerson classified 4 stages ofposterior tibial tendon dysfunction. Flexible flatfoot, which is classified asa stage 2 abnormality, is defined by tendon elongation, with a mobile andcorrectable hindfoot deformity.The accessory navicular (AN) is a supernumerarybone present in 10% to 14% of normal feet. Three types of AN have beendescribed. Type I is present as a small ossicle within the substance of the posteriortibial tendon; type II forms a larger, triangular ossification center adjacent to the naviculartuberosity and connected by a synchondrosis; and type III is a fused orossified cornuate fragment.AN symptoms present as local pain, and, in somecases, an abnormal insertion of the posterior tibial tendon (PTT) onto the ANwill be present. Treatment of the flexible flatfoot with the symptomatic AN isa 2 part procedure that involves correcting the deformity of the flexibleflatfoot and relieving the related symptoms, followed by treating thesymptomatic AN.The aim of treatment of flexible flatfoot deformity is to avoid progressionof the fixed deformity. Surgical techniques have included soft tissueprocedures or osteotomy with medial or lateral column procedures. However,considerable controversy remains regarding which technique will provided thebest outcome. The most common combination of surgical options has been medialdisplacement calcaneal osteotomy (MDCO), combined with some form of PTT augmentation.The second most common combination involves lateral column lengthening (LCL)and PTT augmentation.
Various surgical options are also available for the symptomatic AN,includingsimple AN excision, AN excision and rerouting of the PTT under the navicular,AN excision and restoration of the continuity of the PTT, and arthrodesis ofthe accessory ossicle. A combination of AN excision and PTT reconstruction hasbeen the most commonly used procedure for symptomatic AN. The purpose of thepresent study is to report our experiences and results in patients withflexible flatfoot with symptomatic AN who underwent MDCO with reconstruction ofthe PTT insertion on the navicular bone.
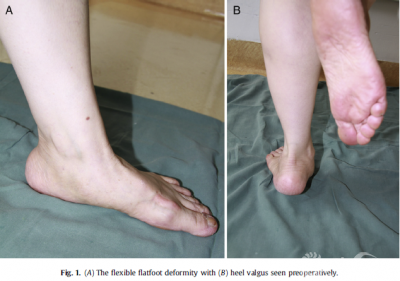
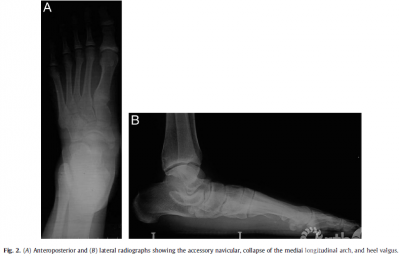
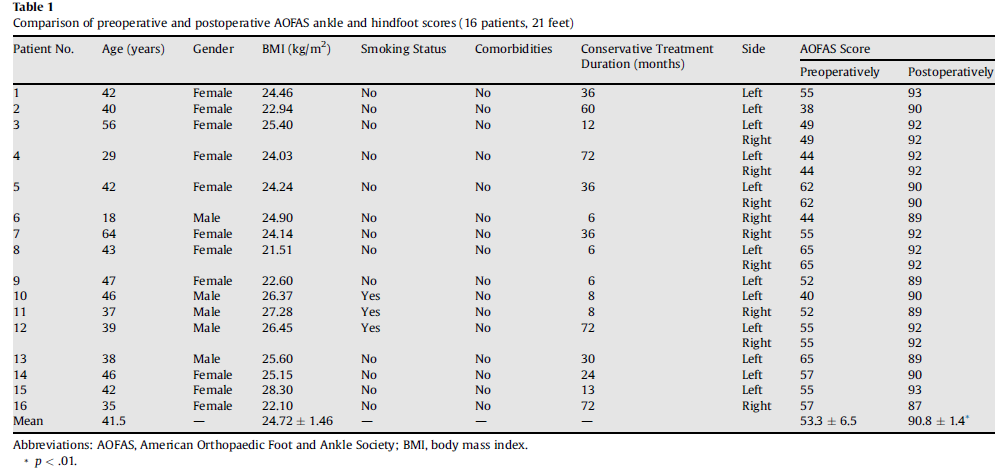
Patients and Methods From December 2008 to July2011, 16 patients (21 feet) with flexible flatfoot,symptomatic AN, and heelvalgus (Fig. 1) underwent MDCO with reconstruction of the PTT on the dorsalnavicular after excision of the AN. All cases were performed by 1 seniorsurgeon at the same hospital. The series consisted of 5 male and 11 female patients,with a mean age of 41.5 years (range 18 to 64years). Of the 16 patients, 11 hadunilateral flatfeet and 5 bilateral flatfeet. All patients had flexibleflatfoot symptoms with a symptomatic AN. The patients presented with chroniclocalized pain on the affected side that made it difficult for them to wearshoes. The presence of flexible flatfoot, AN, and heel valgus were proved radiographically(Fig. 2). Also, T1weighted fat suppressed magnetic resonance imaging showedthat the PTT was abnormally inserted on the AN.
To be included in the cohort, consecutive patients had to haveundergone MDCO with reconstruction of the PTT on dorsal navicular afterexcision of the AN and to have had a minimum of 18 months offollow·up. Additional inclusion criteria were flexible flatfoot, symptomatic AN, and heelvalgus for which conservative treatment had failed,including shoe modification andanti·infiammatory drug therapy for more than 6 months. Furthermore, in allcases, the dysfunction of the PTT, fiattening of the medial longitudinal arch,and heel valgus alignment revealed by clinical evaluation indicated the needfor surgical intervention. However, patients with accompanying seere forefootabduction, multiple arthritis, or infection were excluded from the present study.
Surgical Techniques The patients were placedsupine on the operating table. Spinal anesthesia was given, and a tourniquetwas applied to the proximal thigh. A 3- to 4cm incision was made over the ANto expose the AN and PTT. The AN was excised, and the PTT insertion was fixedon the plantar·medial side of navicular using a 5.0mm suture anchor, applied usinga modified Mason·Allen technique (Athrex, Naples, FL). A lateral skin incision,approximately 4 cm long, was made inferior and parallel to the peroneal tendonsto explore the lateral calcaneal wall. Calcaneal osteotomy was performed frominferiorly and laterally to superiorly and medially, at right angles to thelateral border of the calcaneus. The calcaneal tubercle was medializedapproximately 10 mm, and the osteotomy was stabilized with a 7.3mm cannulatedscrew (Newdeal; Integra, Plainsboro, NJ). The wound was closed, but no cast wasused. All the procedures were performed by 2 senior surgeons (K.L.T., H.H.C.).
Postoperative Management and Evaluation The patients wereimmobilized postoperatively using an XP Walker (Extra Pneumatic, DJOGlobal, St Vista, CA) for 6 weeks. They exercised the leg muscles with isometriccontractions and were prevented from weightbearing movements for 6 weeks.Weightbearing exercise, as tolerated, began after radiographic evidence of consolidationwas seen. Self·directed daily range of motion exercises began at 6 weeks postoperatively.Supervised physical therapy was initiated if a full range of motion had notbeen achieved after 3 months.
The patients wereevaluated preoperatively, 3, 6, 9, and 12 months postoperatively,and every 6months thereafter by 2 senior surgeons (K.L.T., H.H.C.). The clinical examinationincluded assessment of the American Orthopaedic Foot and Ankle Society (AOFAS)ankle and midfoot scores. The radiologic assessments included evaluation of lateraland anteroposterior weightbearing views of the foot and axial views of theheel.The measurements on the lateral weightbearing radiograph of the footincluded the arch height, assessed as the medial cuneiform height, calcaneusinclination angle,talocalcaneal angle, and talar first metatarsal angle. Thetalocalcaneal angle and talar first metatarsal angle wasmeasured on the anteroposterior view of the weightbearing foot radiograph. Heelvalgus alignment was measured on axial radiographs of the hindfoot. Allprevious measurements and assessments were completed by 2 senior surgeons(K.L.T., H.H.C.). The protocol used to manage foot pain, together with the detailsof any operative or postoperative complications, was recorded.
Statistical Analysis Statistical analysis wasundertaken by the operating surgeons (K.L.T., H.H.C.) using SPSS, version 13.0(IBM, Armonk, NY), software. The data were considered in regard to their typeand distribution. Paired Student’s t tests were used to compare the preoperativeand postoperative findings. Values of p ≤ .05 were consideredstatistically significant.
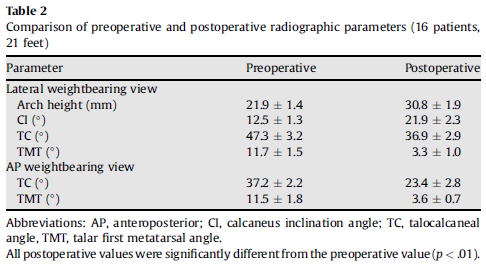
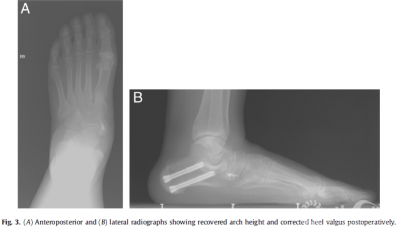
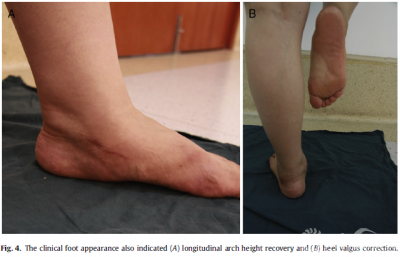
Results The16patients (21 feet)were followed up for a mean duration of 28.5 months (range18 to 48). All patients were satisfied with their clinical results andwere abletowalk long distanceswithout any pain 6 months after surgery. No cases of woundinfection or nerve injury developed.The mean AOFAS ankle and hindfoot scoreshad improved from 53.3±6.5preoperatively to 90.8±1.4 at the last postoperativeassessment(p<.01; Table 1). The improvement in all radiographic parameters wasstatistically significant between the preoperative and last follow·up assessments(p < .01; Table 2). These changes provided evidence of recovery of the archheight and correction of heel valgus (Fig. 3). The foot appearance alsosuggested satisfactory outcomes (Fig. 4).
Discussion Treatment of flexibleflatfoot should include PTT debridement and/or augmentation, LCL, and MDCO. TheLCL corrects the forefoot abduction and hindfoot valgus. However, thedisadvantages of this combination of procedures has included failure to correctfixed forefoot varus, the necessity of using a bone graft to maintain distractionat the site of arthrodesis, and an increased calcaneocuboid joint load.
MDCO is indicated for patients in whom the valgushindfoot deformity is passively correctable and for whom the Achilles tendon canbe directed closer to the normal long axis of the calcaneus to the ground toprotect the medial tendon transfer. This osteotomy will also be effective inrelieving subfibular impingement pain. For the flexible flatfoot, either LCL orMDCO will need to be combined with PTT augmentation.
Thetreatment ofsymptomaticANwill require excisionof theANand PTT reconstruction in many cases.To our knowledge, many surgical options are available, including simpleexcision of the symptomatic AN,the Kidner procedure and its modifications,fusion of the primary andAN bones, and triple arthrodesis. Simple excision ofthe AN can provide satisfactory results for painless physical activity enablingnormal shoes to be worn; however, the procedure does not include PTT reconstructionand fails to correct the flatfoot deformity.
Excision and rerouting ofthe PTT has been shown to provide excellent results, enabling arch recovery;however, the biomechanical effect of the procedure has been reported to beminimal. Fusion of the primary and AN bones will provide reliable healing butcannot remove the medial bony prominence. Arthrodesis has only been used incases of multiple joint arthritis, and no reports have been published of itsuse for the treatment of flexible flatfoot with a symptomatic AN.
In thepresent study, MDCO with augmentation of the PTT was an effective method forcorrecting flexible flatfoot deformity with a symptomatic AN. The PTT wasreconstructed satisfactorily using a suture anchor after AN excision, and good tendon-to-bonehealing appeared to enable quick rehabilitation after surgery.
Just as with mostretrospective observational investigations, we realize that our study wasinfluenced by a number of methodologic shortcomings that could threaten thevalidity of our conclusions,including that the operating surgeons measured theparameters on the radiographs and analyzed the data. However, we did use the AOFASscoring scale for subjective outcome measurements that are known to be reliableand, as such, likely to provide valid information.We believe the use of theAOFAS scoring scale outweighed the known uncertainties related to the influenceof the radiographic measurements on the clinical outcomes.
Heel valgus has been shownto be corrected well using MDCO, with restoration of the gastrosoleal complexas a heel invertor, which increases the supinatory ground reactive forces anddecreases the medial arch load. In our study, flatfoot and heel valgus alignmentwere corrected in all 16 patients. The average longitudinal arch heightincreased from 21.9±1.4 mm to 30.8±1.9 mm, with accompanying improvements in the mean AOFAS ankle andmidfoot scores. All patients were satisfied with their clinical results, andthe procedure was accomplished without complications or infection.Thesatisfactory clinical outcomes in the present study warrant the initiation oflarger studies with longer follow·up to further validate the procedure. Webelieve that the results of our investigation could be useful in thedevelopment of future studies focusing on the surgical correction of the pesvalgus flatfoot deformity.
In conclusion, MDCO withreconstruction of the PTT insertion on the navicular bone is an effectivetreatment of the flexible flatfoot with AN and associated witwith satisfactoryclinical outcomes and correction of the deformity.
转载《The Journal of Foot & Ankle Surgery》
参考文献(略)
作者:Hong-hui Cao,MD 1,Kang-lai Tang, MD, PhD 1,Wei-zhong Lu,MD2, Jian-zhongXu,MD, PhD1
1 Department of Orthopaedic Surgery, Southwest Hospital, ThirdMilitary Medical University, Chongqing People’s Republic of China
2 Department of Orthopaedic Surgery, Traditional Chinese MedicalHospital of Chongqing, Chongqing, People’s Republic of China


 京公网安备11010502051256号
京公网安备11010502051256号